MPD and hip prevention in children
What is this article about?
In this article, we discuss the key points raised in our conversation with Olga Pietryca, a physical therapist who works with children with cerebral palsy (CP). The article focuses primarily on hip problems in children with CP, the importance of early diagnosis, the role of physical therapy, and the collaboration between the entire therapeutic team and the family throughout the treatment process.
- Cerebral palsy and its impact on the motor system
- When should a child with cerebral palsy have their first hip X-ray?
- The GMFCS Scale – How Is a Child’s Functional Level Assessed?
- Surgical treatment – part of a broader process
- Team and family collaboration as the foundation of therapy
- Summary
Cerebral palsy and its impact on the motor system
Cerebral palsy (CP) is a non-progressive disorder of the central nervous system that develops during fetal development or early childhood, for example as a result of strokes. As Olga Pietrzyca points out, one of the main problems in these children is spasticity, or increased muscle tone. This leads to muscle imbalance, in which the flexor and adductor muscles dominate, which directly affects joint alignment, particularly in the hips.
Why are the hips so vulnerable to injury in MPD?
The interview explained that the hips of children with CP are particularly prone to deformities because their proper development depends on movement and weight-bearing. In healthy children, the hip socket gradually takes shape, whereas in CP—due to limited standing and the absence of typical stages of motor development—this process is disrupted. As a result, the acetabulum may remain too steep, and the femoral head begins to gradually displace, leading to hip subluxation or dislocation. These changes are assessed on X-rays, including using the Reimers index.
When should a child with cerebral palsy have their first hip X-ray?
According to these recommendations, the first hip X-ray should be performed between 12 and 18 months of age in children with MPD. Regular monitoring is crucial, as it allows for the early detection of abnormalities and the initiation of treatment before serious deformities develop. In practice, however, there are situations in which children go for many years without undergoing imaging diagnostics, even though it should be standard practice in the care of patients with MPD.
The GMFCS Scale – How Is a Child’s Functional Level Assessed?
The interview also explained the significance of the GMFCS scale, which is used to classify the functional level of children with CP. The scale has five levels—ranging from children who move almost like their healthy peers to children who are completely dependent on caregivers for daily functioning. This assessment helps specialists select the appropriate treatment strategy, rehabilitation, and orthopedic equipment tailored to the child’s actual capabilities.
The Role of Physical Therapy and Parents in Daily Treatment
As Olga Pietrzyca emphasizes, physical therapy for children with cerebral palsy doesn’t end in the therapy room. Parents play a key role by continuing the therapy at home. Important elements of daily care include standing, regular stretching, and the use of equipment such as standing frames. It is recommended that children spend time standing for about 45 minutes, even twice a day. It is precisely this consistency and the family’s commitment that have a huge impact on the results of therapy.
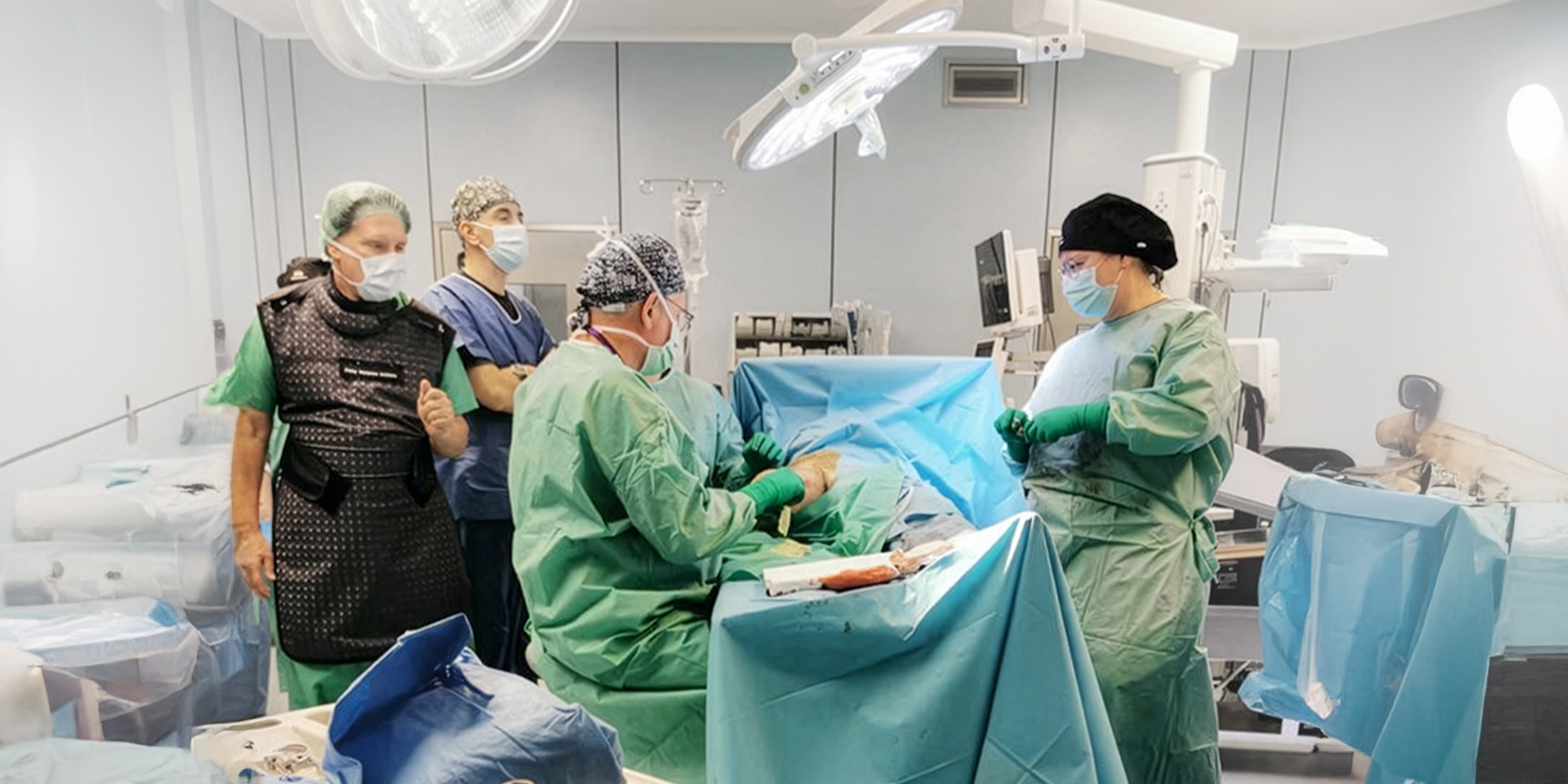
Surgical treatment – part of a broader process
In cases of advanced hip disease, surgical treatment becomes necessary; however, as emphasized in the podcast, this is not a single procedure but an entire process. It includes preoperative preparation, decisions made by a multidisciplinary team, and intensive postoperative rehabilitation. There is an increasing shift away from prolonged immobilization toward early mobilization of the patient within the first few days after surgery, which allows for faster restoration of function and reduces complications.
Team and family collaboration as the foundation of therapy
The treatment of children with cerebral palsy requires close collaboration among many specialists—physical therapists, orthopedists, and neurologists—as well as the active involvement of the family. As the interview reveals, only a team-based approach allows for effective treatment planning, monitoring of progress, and responding to changes in the patient’s condition. The child is always at the center, but their therapy also involves the parents and the entire support network, which plays a key role in the rehabilitation process.
Summary
MPD is a complex condition that requires early diagnosis, regular monitoring of the hips, and consistent rehabilitation. It is crucial to perform the first X-ray at the right time, to provide systematic physical therapy, and to ensure that the entire treatment team works closely with the child’s family. As the podcast explains, only a comprehensive and long-term approach offers the best chance of improving the functioning and quality of life for children with MPD.