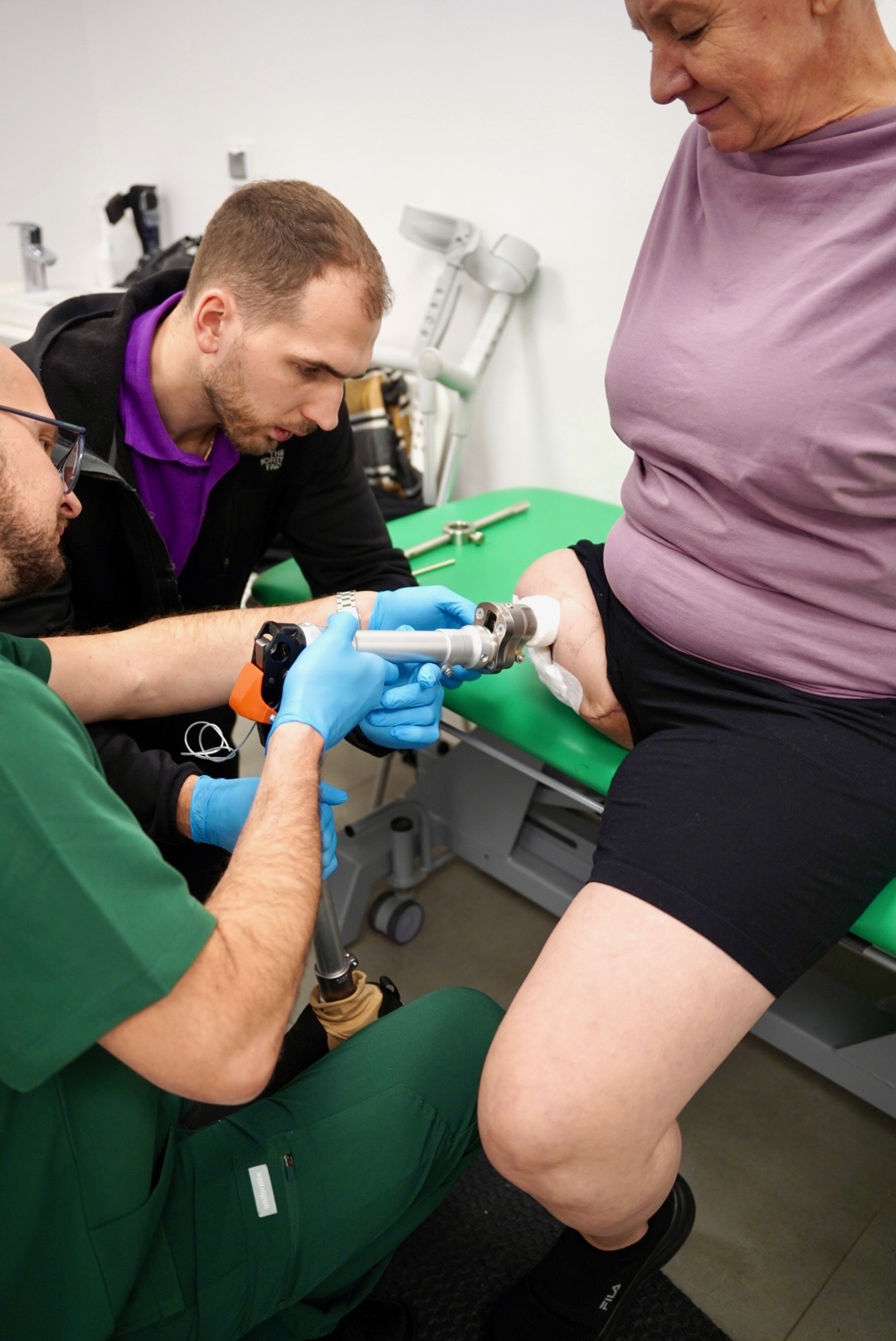
Single-Stage Osseointegration – A Breakthrough in Prosthodontics at the Paley European Institute in Warsaw
Regain your mobility, freedom of movement, and a full sense of the ground beneath your feet, thanks to the direct connection between the prosthesis and the bone.
Osseointegration is a modern prosthetic method that eliminates the need for a traditional prosthetic socket. Instead of attaching the prosthesis to the residual limb, you secure it directly to an implant embedded in your bone. This solution restores a quality of life to amputees that they could previously only dream of
Discover the benefits of a denture without a base
Traditional prosthetic solutions rely on directly attaching the socket to the skin of the stump, which often causes discomfort and painful chafing and does not provide stability. Osseointegration (from the Latin os – bone, integratio – joining) is a groundbreaking method in which a titanium implant permanently fuses with living bone tissue, becoming an integral part of your body.
Why choose osseointegration?
Natural sensation (osseoperception): Thanks to the direct connection to the bone, you’ll begin to “feel” the ground beneath your feet. Vibrations are naturally transmitted from the ground to the bone, and you’ll also “feel” the prosthesis’s position in space. You can walk backward in dark rooms without looking down at your feet.
Excellent prosthesis stability: you gain full control over rotational movements, and the stump no longer slips out of the socket.
No more skin problems: Completely eliminating the traditional stoma bag eliminates the problem of chafing, painful pressure, abrasions, changes in stump volume, and excessive tissue sweating.
Full range of motion: The absence of a rigid shell around the stump allows for a full range of motion in the joints (hip or knee). The joints align properly, which improves stability and prevents contractures. Your movements become smooth and natural.
Instant fitting: Thanks to the intuitive connector, it takes just a few seconds to attach and remove the denture.
Greater stability and strength: The load is transferred directly to the skeleton, which prevents bone loss and strengthens the muscles.
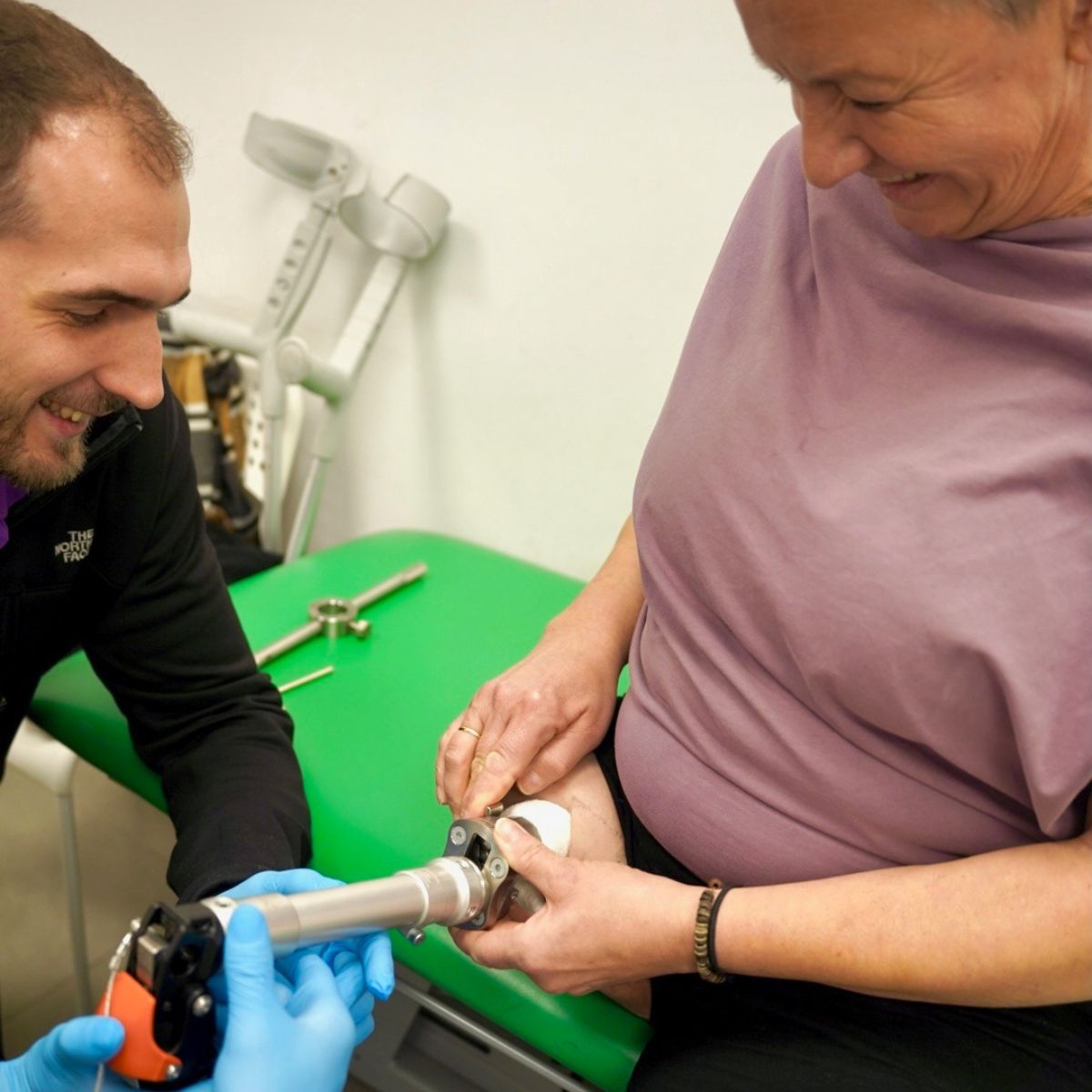
One-stage osseointegration
At the Paley European Institute, we use the OPL (Osseointegrated Prosthetic Limb) implant—the world’s first implant designed specifically for single-stage procedures, which has been refined over the past 15 years.
Our treatment follows the Osseointegration Group’s surgical and rehabilitation protocols—including the press-fit implantation technique, muscle group balancing, and stoma reconstruction—which allow for loading of the implant and the start of rehabilitation as early as the first day after surgery.
Numerous clinical studies and publications have confirmed that, thanks to state-of-the-art OPL engineering and standardized surgical and rehabilitation protocols, complications—including infections—have been minimized, and full weight-bearing and gait retraining have been significantly accelerated.

Osseointegration: A Life Without Limitations After Amputation
Regain natural control over your movement with technology that fuses the implant directly to your bone.
Osseointegration is a groundbreaking alternative to traditional prosthetic methods. Instead of the pressure and painful friction caused by a denture base, we offer stable, secure denture retention using an implant permanently fused to the bone. At the Paley European Institute, we restore what is most precious to our patients: confidence in their step, a sense of the ground beneath their feet, and the comfort of everyday life. Our standard of care includes:
Personalized assessment: We analyze your anatomy and medical history to find a solution that’s perfectly tailored to your body and lifestyle.
International Surgical Protocol: We use advanced, internationally proven implant placement techniques to minimize the risk of complications.
Biomechanical integration: We ensure that your bone and the implant fuse together, providing a stable foundation for the prosthesis.
Specialized rehabilitation: We guide you step by step through the process of learning to walk and putting full weight on your limb under the supervision of experts.
Why is this a breakthrough? Moving away from traditional external fixation marks the definitive end of problems typically associated with the hip socket and restores the joint’s full, natural range of motion.
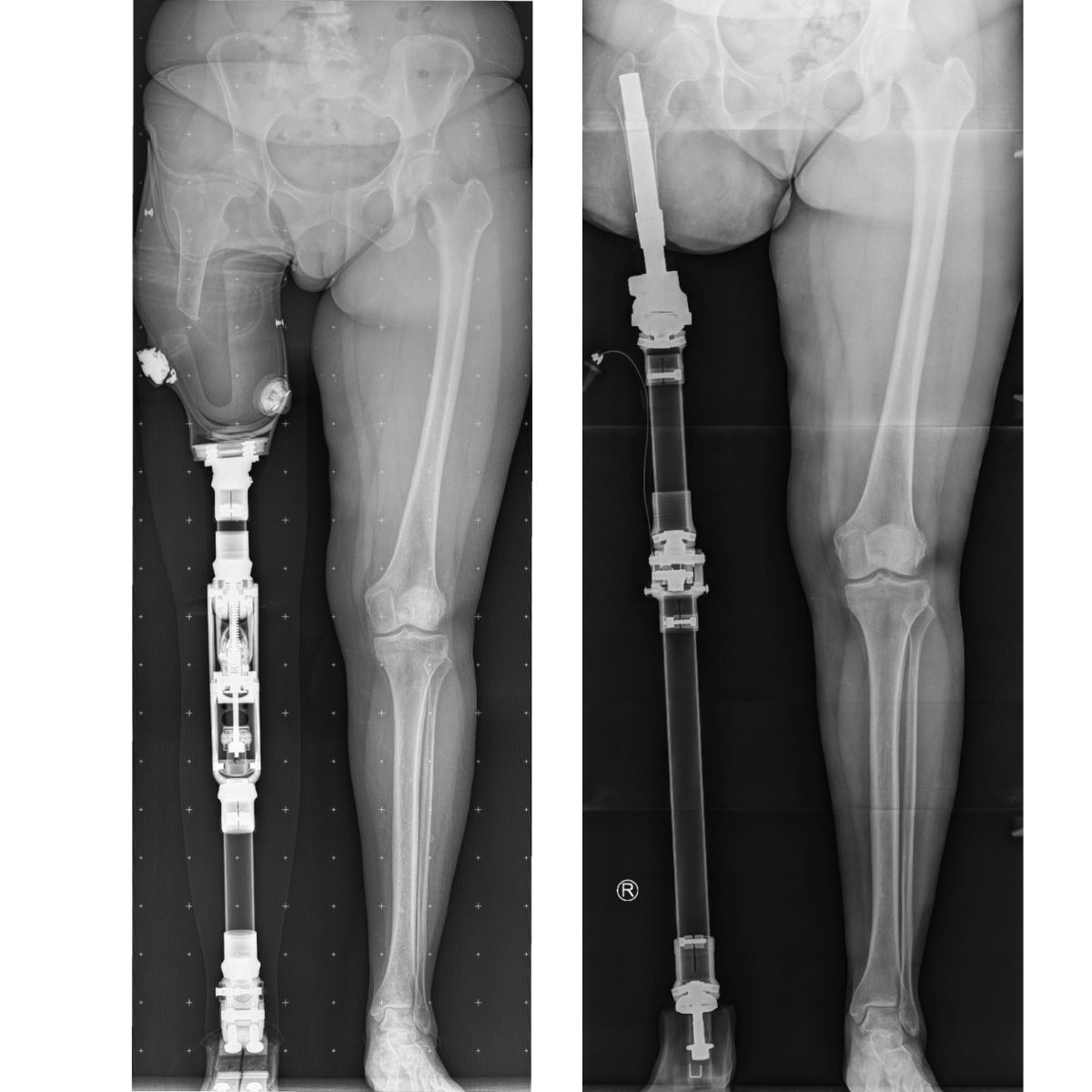
Who is osseointegration for?
When conventional dentures fail...
If a traditional denture base limits your mobility, causes pain, or leads to recurring skin problems, osseointegration is the solution for you. This method is particularly effective for patients with short residual limbs and challenging anatomical conditions, where conventional dentures are impossible or uncomfortable.
Safety Guarantee: Comprehensive Qualification
Your journey to a new level of fitness at the Paley European Institute begins with a thorough assessment. Our evaluation process is a multidisciplinary approach that includes:
A comprehensive orthopedic consultation: A thorough review of your medical history and your functional goals.
Consultation with a team of physical therapists: Assessment of biomechanics and motor potential.
Psychological support: Professional guidance to help you adjust to your new lifestyle with a new type of prosthesis.
Advanced gait analysis: Objective parameters that allow us to plan an optimal treatment regimen.
Prosthetic consultation: selecting denture components to maximize function and ensure they meet your individual needs and expectations.
Long-term success and a proprietary care model:
When you choose osseointegration at our Institute, you are opting for a proven, comprehensive system. We combine world-class surgical procedures with a personalized rehabilitation plan and a long-term care plan. This approach ensures a lasting improvement in your quality of life and the full, safe integration of the implant with your body; you become part of the “Paley Family” for many years to come.
Clinical indications
Amputation of a lower limb (thigh or lower leg)
Intolerance to traditional dentures
Chronic wounds, abrasions, and stump ulcers
Severe pain caused by pressure on the funnel
Instability and lack of full control over the prosthesis
Patients eligible for amputation due to neuropathic pain and other causes
On a case-by-case basis: following upper limb amputation, joint dislocation, or other complex conditions
Patient Profile
People with a short stump (which is difficult to fit with a prosthesis)
Patients who have undergone bilateral amputation
Patients striving for an active lifestyle
People who experience discomfort when sitting in a prosthetic limb
Patients who have undergone unsuccessful conventional treatment
People looking for a natural sense of the ground (osseoperception)
The PORT Approach to Osseointegration Treatment
A harbor is a safe haven, a place where we can finally catch our breath or prepare for the next storm.
The PORT approach is a proprietary, structured model of care for amputees that ensures safety and the highest quality of life at every stage—from preoperative preparation through to long-term support.
Here are the updated, professional guidelines for each phase of the PORT model, based on the latest medical standards from the Paley European Institute:
Prehabilitation (Rehabilitation and Preparation)
Objective: Biological and psychophysical optimization prior to the procedure.
Multidisciplinary evaluation: Comprehensive medical and functional assessment of a candidate for dental implant surgery.
Treatment planning: A meeting with the team (surgeon, physical therapist, psychologist, prosthetist) to discuss a personalized treatment plan.
Optimizing health: Preparing the body for implantation to minimize the risk of infection and ensure implant stability.
Education and Preparation: Establishing realistic patient expectations and providing the psychological support necessary to perform the procedure.
Preoperative rehabilitation: A 2-week intensive program designed to prepare patients physically and psychologically for surgery and to optimize the postoperative rehabilitation process.
Osseointegration (Surgery and Integration)
Objective: Precise implantation and initiation of biological integration.
Reconstructive surgery: The procedure is performed by an experienced team at a specialized limb reconstruction center.
Safety standards: The use of standardized and technically consistent surgical protocols.
Care coordination: Continuous medical supervision and support from a dedicated coordinator during hospitalization.
Pain Management: Advanced methods for controlling postoperative pain to ensure maximum patient comfort—“ZERO PAIN PROTOCOL”—aimed at minimizing neuropathic complications commonly seen in amputees.
Rehabilitation (Rehabilitation and Healing)
Objective: Gradual loading of the implant and learning to walk.
Early mobilization: Immediate implementation of a globally unique, safe, and controlled implant loading protocol that accelerates osseointegration.
Interface protection: Gradual increase in pressure and controlled intensification of exercises under the supervision of a physical therapist to prevent implant loosening and stoma damage.
Functional training: Learning how to use a new prosthesis safely and restoring proper movement patterns.
Healing monitoring: Continuous clinical monitoring of the integration process and the condition of soft tissues.
Training & Long-Term Care
Goal: Return to full activity and lifelong follow-up.
Advanced gait training: Structured improvement of functional mobility and movement dynamics.
Social reintegration: Support for returning to professional, social, and athletic activities (para-sports).
Lifetime Follow-Up (Term): Regular monitoring of the implant’s condition, prevention of complications, and lifelong prosthetic care.
Psychological adjustment: Ongoing support to help you fully realize the potential of your new mobility and improve your quality of life.
Osseointegration vs. Traditional Overdenture – Which Should You Choose?
Learn about the differences in biomechanics, comfort, and daily activities that determine your mobility after an amputation.
Osseointegration
's natural gait pattern
The load-bearing forces act directly on your bone. Thanks to axial weight transfer, you gain stability, precision of movement, and full control over your prosthesis without any extra effort.
Lower energy expenditure
Muscles and joints work in a natural position and through their full range of motion. The residual limb does not sink into the socket, and you don’t have to lift your limb excessively to move the prosthesis during a stride. You conserve energy, tire less easily, and cover longer distances.
’s Unique Osseoperception
Once again, you can “feel” the surface beneath your feet. The vibrations transmitted by the implant to the bone allow you to distinguish between asphalt and grass, which dramatically improves your safety and balance.
Maximum comfort and skin health
With no socket, say goodbye to pressure issues, painful chafing, and skin irritation. Your prosthesis fits perfectly every day, regardless of any swelling or weight fluctuations.
Complete freedom in everyday life
You can sit down comfortably (full 90° flexion), which is essential in the car or at the office. Attaching and detaching the prosthesis takes just seconds, allowing you to stay active all day long.
Easy hygiene and freshness
Your skin "breathes" naturally. Maintaining the connector is quick and easy, eliminating the problem of excessive sweating and unpleasant odors typical of closed systems.
Classic funnel denture
Stress on Soft Tissues
Your body weight rests on the skin and muscles of the stump. This leads to chronic pain, pressure on nerves, prosthesis instability, and rapid fatigue while walking.
The bone is not directly loaded, which leads to a loss of bone quality and osteoporosis.
Abnormal joint alignment
The joints above the socket are often misaligned, leading to contractures, limited mobility, early degenerative changes, and reduced muscle function.
Lack of Ground Feel (Insulation)
The thick layer of foam and silicone liner isolates you from your surroundings. You can’t feel the ground, which forces you to constantly watch your step and increases the risk of tripping.
Risk of Stump Damage and Injuries
Constant skin contact with a hard socket promotes the development of painful pressure sores and inflammation. This often requires costly and time-consuming adjustments.
Limited mobility and discomfort
The stiff rim of the socket digs into the groin or buttock when sitting, causing numbness. The process of putting on the prosthesis is cumbersome and requires the use of lubricants. Changes in stump volume (swelling) over the course of a day, menstrual cycle, pregnancy, weight fluctuations, or air travel make it difficult to adjust the socket.
Hygiene and Sweating Issues
A tight seal between the stump and the socket causes excessive sweating and tissue maceration. This creates an ideal environment for bacteria and fungi, which often leads to skin infections.
The osseointegration treatment process includes:
Each case eligible for osseointegration is evaluated individually by a multidisciplinary team. Treatment does not end with surgery—it includes preparation, the procedure itself, controlled integration of the implant with the bone, as well as standardized rehabilitation and long-term prosthetic, orthopedic, and therapeutic care.
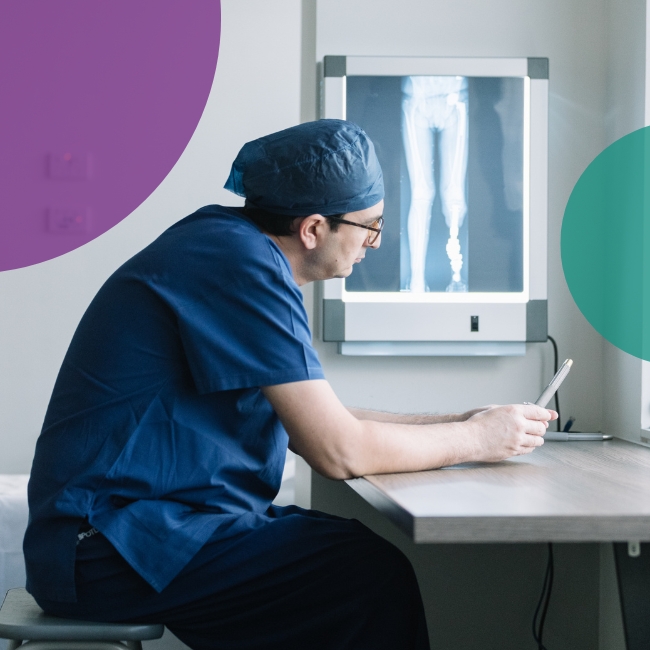
Assessment and Diagnosis
The first step involves a detailed orthopedic consultation and a review of the patient’s medical history. Imaging tests (CT scans) are performed to assess the quality and length of the stump, the diameter of the medullary canal, and the anatomical conditions. Patients may also undergo a psychological consultation to help them prepare for the treatment process and adapt to osseointegration.
Based on this, the team evaluates the indications, potential risks, and the feasibility of a one-stage osseointegration procedure.
In addition, the physical therapy team performs functional assessments and, for ambulatory patients, gait analysis as well.
Procedure Planning
Using 3D analysis (three-dimensional reconstruction) of CT scans, we can select the ideal implant size for the patient’s bone.
We determine the surgical strategy and any additional surgical procedures (soft tissue reconstruction of the stump, nerve surgery, etc.) as well as the pain management protocol.
The plan also includes a rehabilitation schedule and a detailed discussion with the patient regarding the subsequent stages of treatment, the recovery period, and safety guidelines.
In cases requiring reconstructive preparation (e.g., treatment of infections, stump correction), a phased treatment plan is established.
To boost self-confidence and reduce anxiety, patients can participate in a two-week preparatory program, during which they will meet other patients who have undergone amputations (and sometimes osseointegration), improve their physical condition and fitness, and learn exercises to perform after surgery.
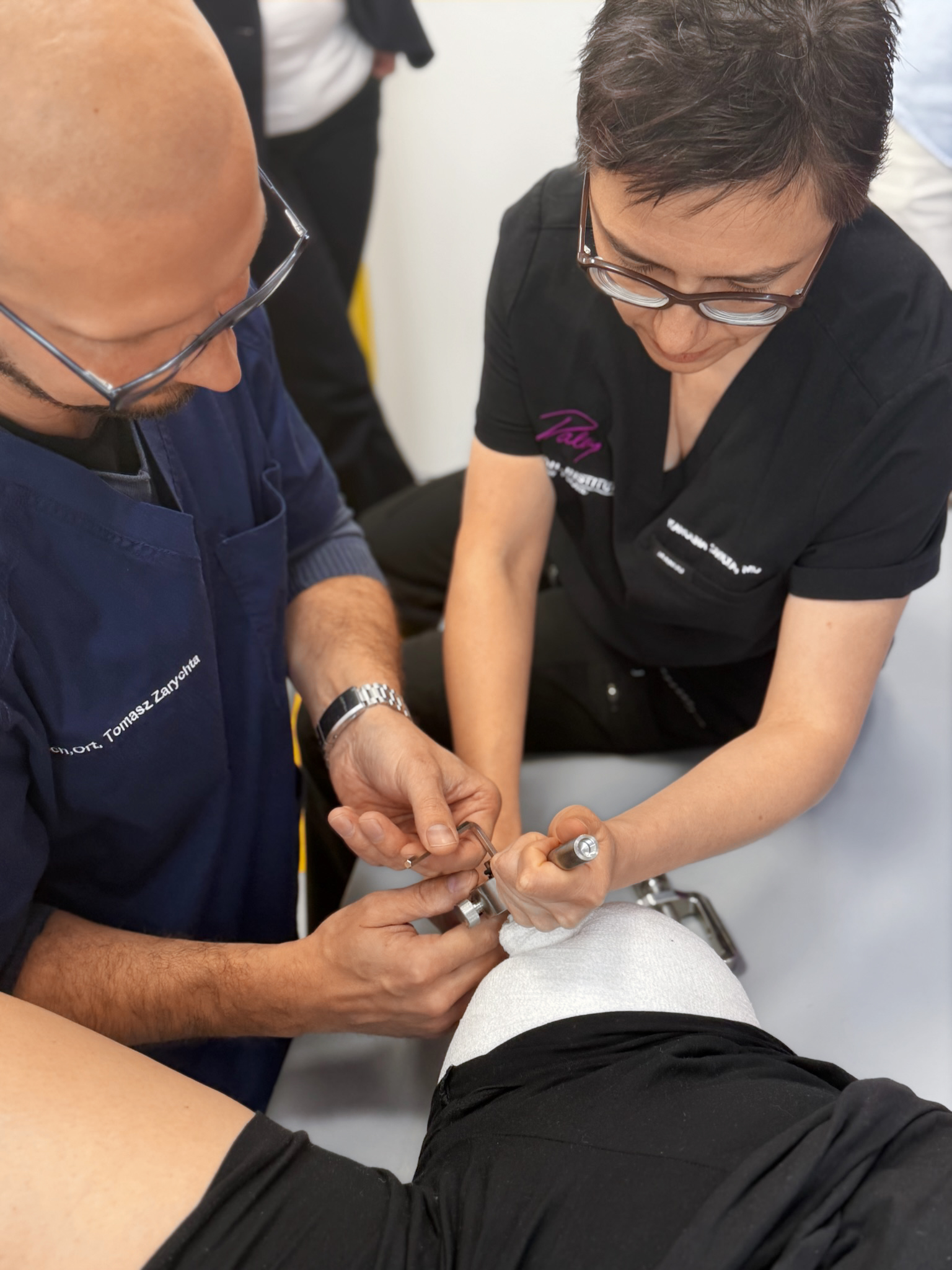
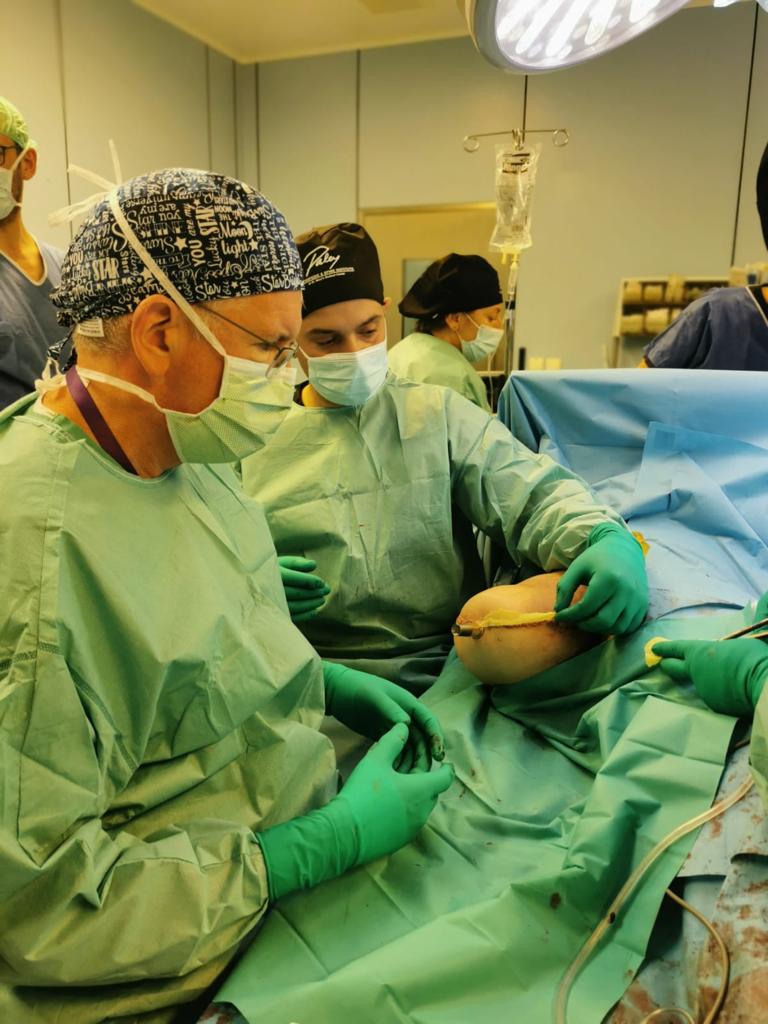
Operation
The procedure involves inserting an implant into the bone, securing it in place, and bringing the connector through the skin.
In a one-stage procedure, the implant is placed and the abutment is attached during a single surgery. In certain cases, a two-stage procedure is used.
The hospital stay is relatively short, and the patient remains under the constant supervision of the Paley European Institute’s pain management, surgical, and physical therapy teams.
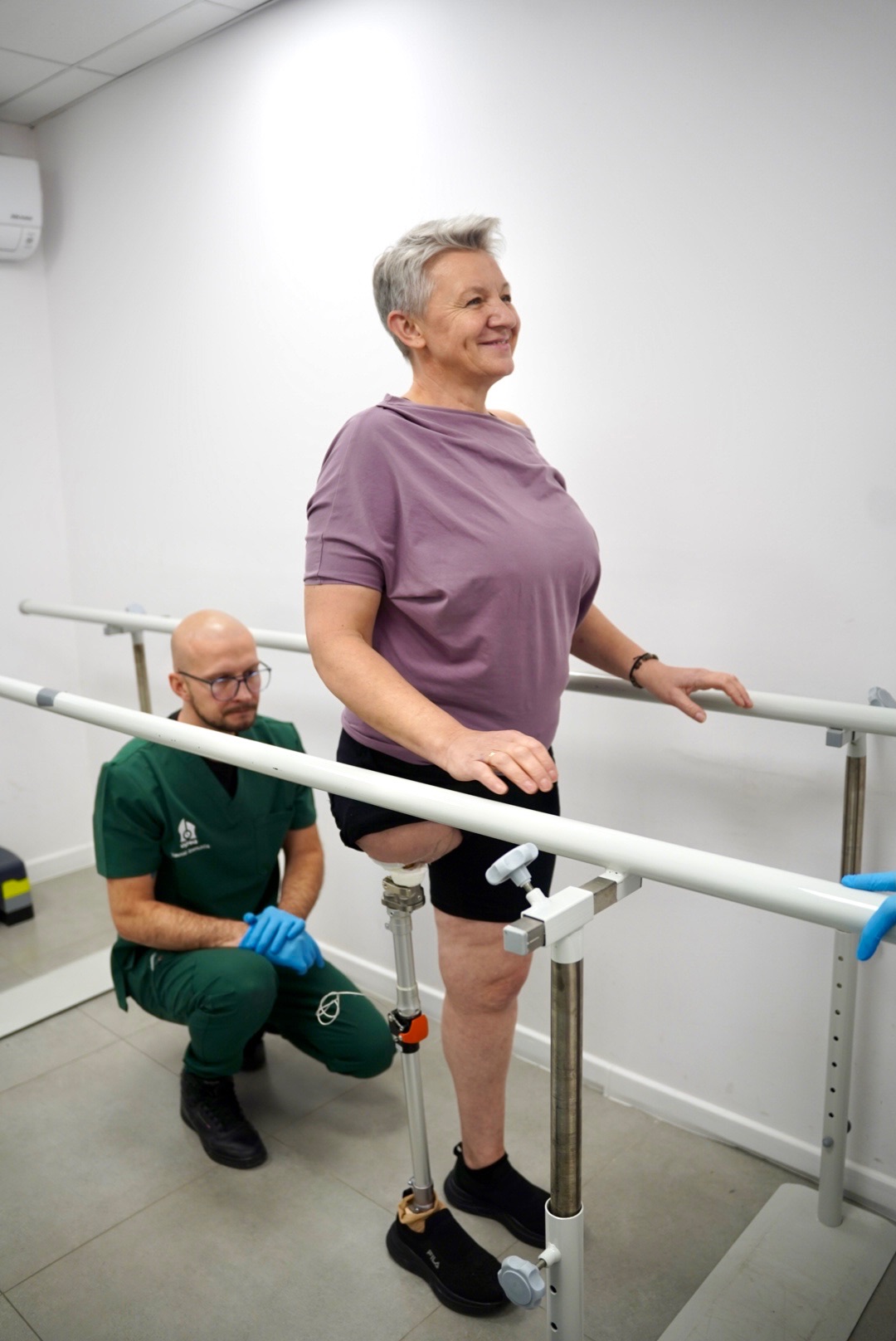
Orientation and rehabilitation period
After surgery, a crucial phase begins: controlled mechanobiological adaptation.
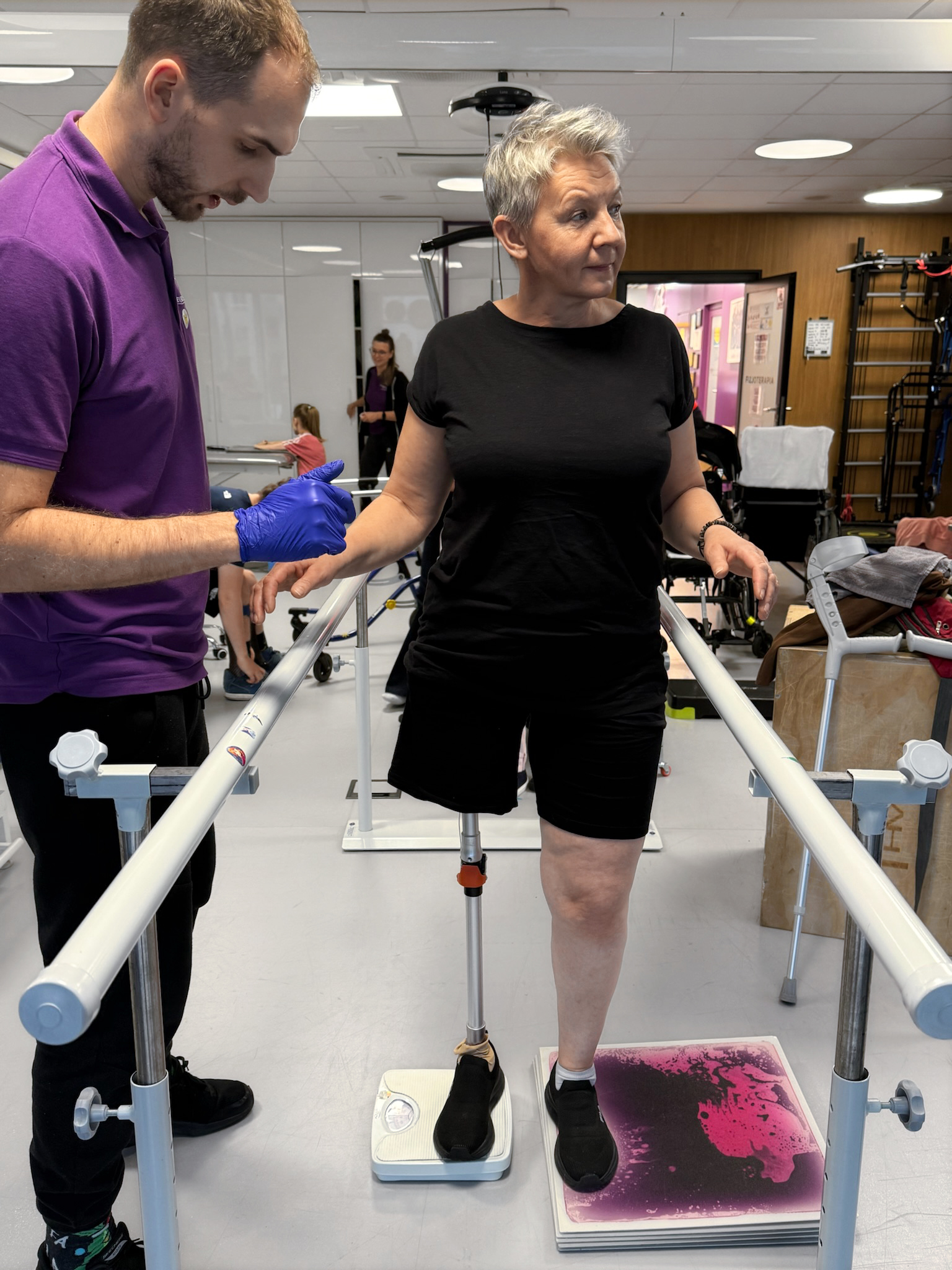
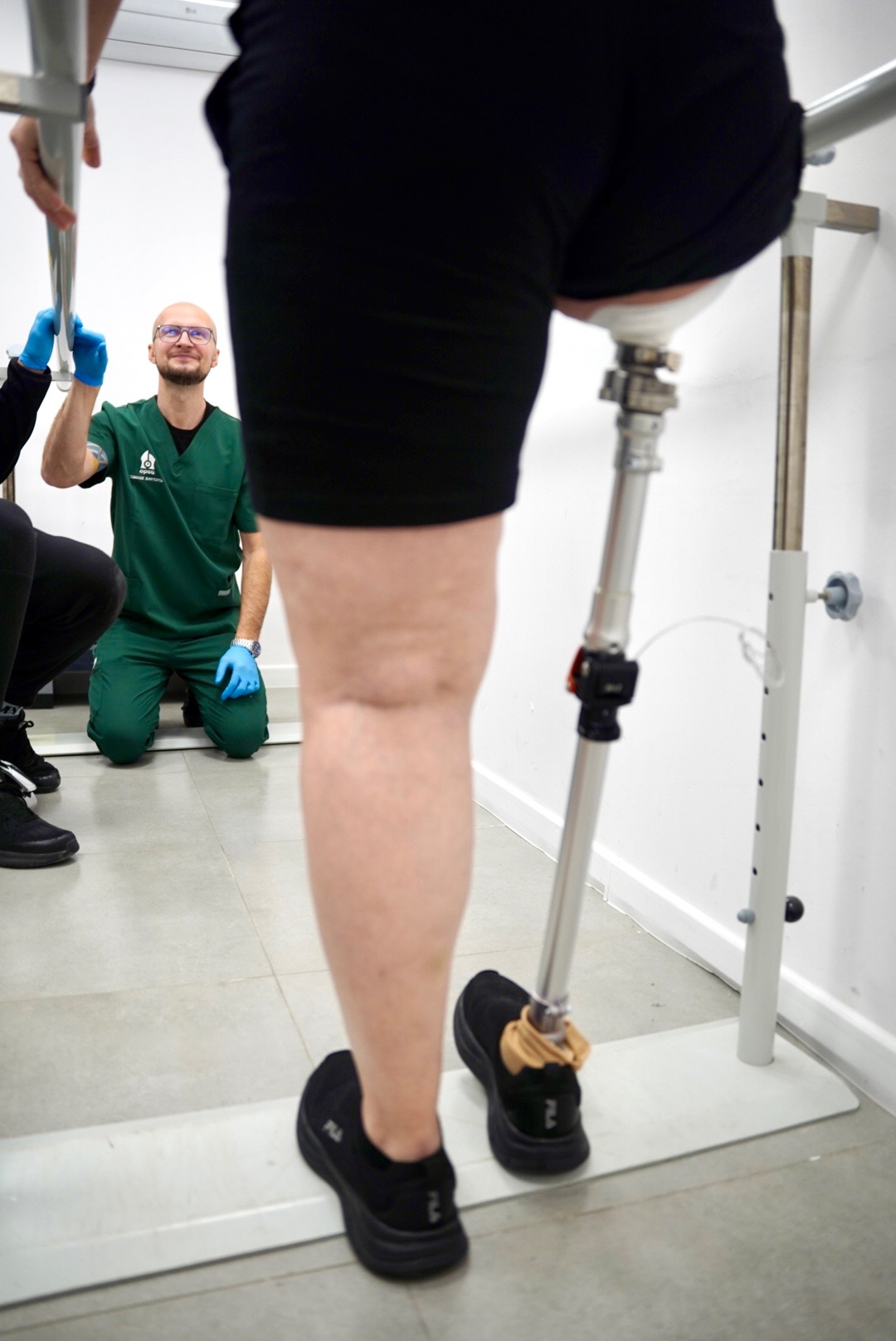
The implant gradually integrates with the bone, while the patient follows a standardized rehabilitation protocol that includes progressive weight-bearing on the limb, fitting with a training prosthesis, and gait training.
Regular clinical and imaging examinations allow for monitoring of the integration process and treatment safety.
Prosthodontics
Once the integration phase is complete, the external prosthesis is fully adjusted and the patient’s range of motion is expanded.
The patient regains greater stability, improved axial sensation, and the ability to move more naturally.
The treatment process does not end at the time of activation—it includes long-term follow-up care and the option to replace OPL system components and prosthetic components.
We are part of the Osseointegration Group (OG)
We are a proud partner of a global network of leaders in osseointegration, which gives our patients access to expertise based on over 900 successful cases (successful OPL system implantations / satisfied patients successfully treated with the OPL system) worldwide.
The Foundation of Professional Knowledge (OG Legacy)
Our collaboration with the Osseointegration Group and Prof. Munjed Al Muderis is the foundation of our work.
OG is an elite group of specialists that has revolutionized the lives of amputees by establishing standards that are now used worldwide.
Access to global statistics and innovations from the
Our approach is based not only on our own clinical experience, but also on years of analysis of treatment outcomes at Osseointegration Group partner centers and other leading osseointegration centers around the world. We collaborate with specialists from Australia, Europe, and the Americas, which allows us to continuously update our protocols. We use the latest registered OPL implant system, which is also used in other reference centers.
’s Global Model of Comprehensive Care
Our collaboration ensures that patients follow a standardized pathway: from precise evaluation, through innovative surgery, to unique rehabilitation. This approach allows us to achieve the highest levels of effectiveness and safety while maintaining a personalized approach.
Paley European Institute: A global standard in Poland
As an integral part of the Paley Institute’s global network, we provide access to the most advanced osseointegration systems, based on standardized and proven medical protocols.
A global network, one standard (Unified Protocol)
We operate within the strict framework of the Paley Institute, which means that every stage of your treatment—from the initial consultation to the final rehabilitation—follows the same rigorous guidelines as in our centers in the U.S. and the United Arab Emirates.
Direct Expertise from the Pioneers
Our team, led by Dr. Karolina Siwicka, MD, PhD, directly carries on the legacy of Prof. Munjed Al Muderis. Dr. Siwicka is implementing her own surgical techniques in Poland, which have revolutionized modern osseointegration worldwide.
Certified safety and innovation
We use only genuine, clinically proven, and CE-certified OPL implants. Thanks to the constant exchange of expertise within our network, we follow up-to-date protocols based on medical evidence, so you can be confident that your treatment is in line with the latest scientific knowledge and is performed in a predictable and consistent manner.
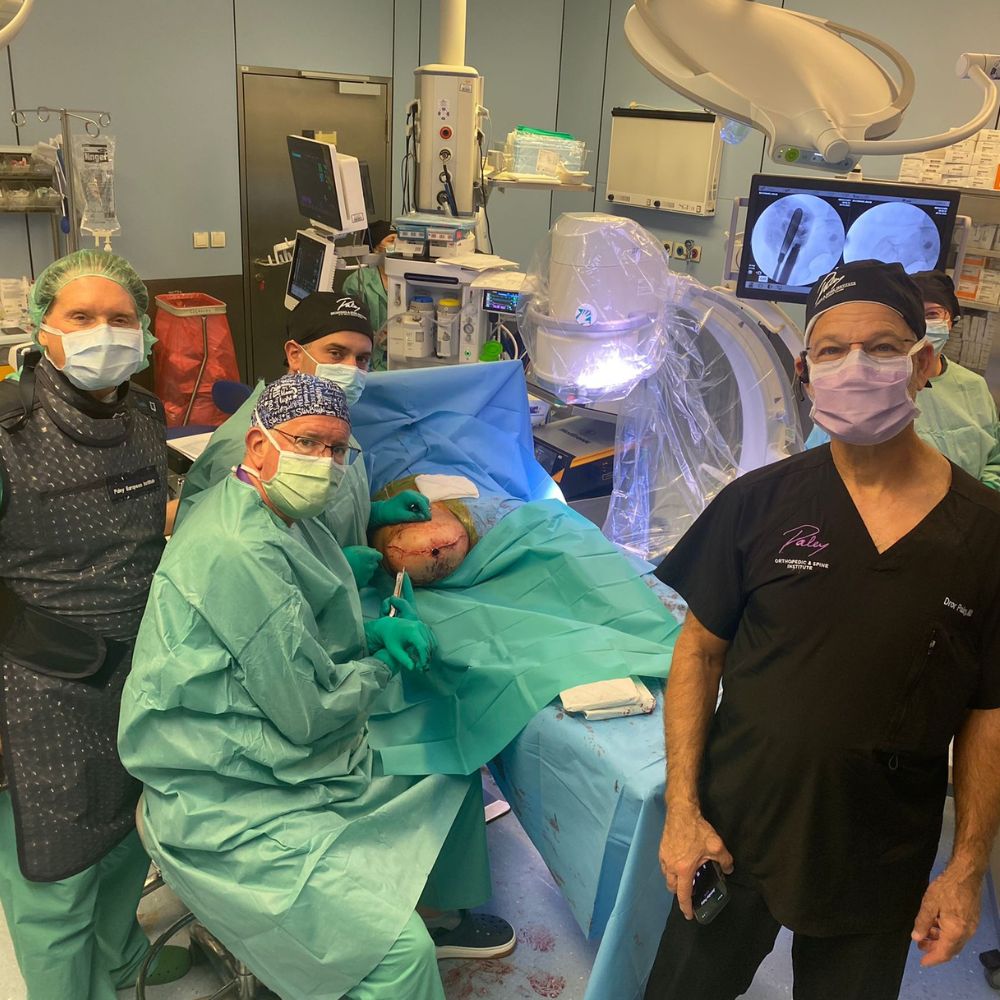
Karolina Siwicka, M.D., Ph.D. – reconstructive surgeon, orthopedic surgeon, and musculoskeletal traumatologist.
Dr. Karolina Siwicka, Chief Physician of the Osseointegration Program at the Paley European Institute, is one of the few specialists in the world who combines expertise in complex reconstructive surgery with pioneering knowledge in the field of osseointegration. As a key pillar of the Institute, she serves as the leader of the team dedicated to restoring mobility to patients following limb amputations.
A global career path: 4 continents and 20 years of experience.
Dr. Siwicka honed her unique expertise at the world’s most renowned orthopedic centers, learning directly from the visionaries of modern medicine:
Australia – a colleague of Prof. Munjed Al Muderis: At a leading Australian center in Sydney, Dr. Siwicka co-led groundbreaking research on the safety of osseointegration. She observed that this method represents a breakthrough for patients with diabetic foot, significantly reducing their post-amputation mortality rate and accelerating their return to independence.
Japan – She spent nearly six years there, working in the departments of pediatric orthopedics, hand surgery, and foot reconstruction. She earned her Ph.D. in limb lengthening and conducted advanced research on bone regeneration in patients with achondroplasia.
Africa – As a fully qualified specialist, she treated the most difficult cases of bone deformities and infections at the only pediatric orthopedic hospital in Malawi. In Cape Town, she specialized in limb reconstruction and the Ilizarov method.
Italy – During her two years of medical studies in Italy, she completed numerous clinical internships at local reconstructive surgery centers. Her treatment philosophy has always been: "Less is more." In her practice, Dr. Siwicka adheres to the principle of maximizing functionality while minimizing the burden on the body.
"Osseointegration isn't just a procedure—it's an opportunity to regain 99% of who you were before the amputation. My goal is to guide the patient through this process in a safe and predictable manner."
Osseointegration by the numbers
Global Scale and Experience
Over 900 OPL osseointegration procedures performed at partner centers worldwide
More than 650 patients who have regained their mobility and quality of life thanks to this method
20 years of clinical experience – the first integrated lower-limb prosthesis was introduced in 1999
12 medical centers worldwide that actively perform osseointegration procedures using OPL implants, including prestigious facilities in Sydney, London, Rotterdam, and Warsaw
Efficacy and Safety
>98% success rate among patients undergoing the procedure
Less than 2% – overall revision rate for the femur (most commonly due to septic loosening or lack of integration)
A 100% improvement in quality of life reported by patients after switching to a leadless system
Time and Rehabilitation (OGAAP-2 Protocol)
3–6 weeks – the total duration of surgery and physical therapy required to regain independence under a standard single-stage protocol
Less than 10 seconds —the time it takes a patient to insert or remove an osseointegrated prosthesis on their own
3 months – the average time after which most patients stop using crutches and begin walking on their own
Amputation Statistics and Needs
There are currently more than 30 million people worldwide who have undergone an amputation (according to WHO estimates)
2,000 amputations are performed each year in Poland alone
70% of amputations result from complications of diabetes and peripheral vascular disease (PVD), which, thanks to modern research, are no longer a contraindication for osseointegration
Our Doctors Meet the Paley European Institute team
Our Partners on the Path to Fitness
The success of osseointegration treatment relies on close collaboration between world-class engineers, experienced surgeons, and specialized physical therapy teams. At the Paley European Institute, we join forces with industry leaders to ensure our patients have access to the safest and most innovative technologies in the world. Each of our partners supports the recovery process at a different, critical stage—from precise implantation and perfect prosthesis fitting to mental and social support.

Osseointegration International is a global pioneer and provider of the most advanced implant systems used in bone-free surgery. The company offers certified solutions that enable a direct, stable connection between the prosthesis and the patient’s skeleton. Thanks to ongoing research and collaboration with leading surgeons (including Prof. Munjed Al Muderis), these implants are characterized by the highest biocompatibility and durability, serving as the foundation for restoring a natural gait pattern and unique osseoperception.
Read more: https://osseointegration.org

OPSA (Orthotic and Prosthetic Specialists Association) is an elite team of prosthetists, orthotists, and engineers specializing in state-of-the-art prosthetic solutions for patients following osseointegration procedures. Their role is to create a personalized limb prosthesis compatible with the OPL system, which works perfectly with the patient and meets their functional expectations. The OPSA team closely coordinates its activities with surgeons, physical therapists, and engineers, ensuring that every prosthesis provides maximum freedom of movement, comfort, and natural dynamics during daily activities.
Read more: https://opsa.pl/o-firmie/#

The Znowu w Biegu Foundation is a key partner in the process of returning to full social integration and physical activity following an amputation. It offers comprehensive rehabilitation programs and psychological support. It helps candidates for osseointegration prepare for surgery and then supports them as they adapt to life with their new prosthesis. In collaboration with medical teams, it creates a safe space where patients can build a new identity, regain self-confidence, and gradually return to sports activities and professional pursuits.
Read more: https://znowuwbiegu.pl
Multimedia
A patient- and family-centered approach
Osseointegration treatment is not just a surgical procedure, but also a process that requires support on many levels—physical, emotional, and social. That is why at the Paley European Institute we use a Family-Centered Care model, in which the patient and their loved ones are an active part of the entire treatment process.
A team of specialists—including surgeons, physical therapists, psychologists, and prosthetists—works together to provide comprehensive care before surgery, during treatment, and throughout rehabilitation. Patients and their families receive clear information about every stage of treatment, which helps them make informed decisions and reduces the stress associated with treatment.
We also place a strong emphasis on psychological support and preparing the patient to live with a prosthesis following osseointegration. This ensures that the adaptation process proceeds safely, allowing the patient to gradually regain independence and confidence in their daily activities.
This approach allows us to take a holistic view of treatment—not just as a surgical procedure, but as a path to improving the quality of life for the patient and their family.
Challenges, perseverance and hope
Read about our patients
The Story of Jacob
LIVE + Q&A with The Osseointegration Group
Your most frequently asked questions
That is, What you as a parent should know before making a decision.
Osseointegration involves the surgical placement of an implant into the bone, which then fuses with the bone during the healing process. This creates a stable, direct connection to the prosthesis, eliminating the need for a prosthetic abutment.
Safety depends on the team’s qualifications and experience, as well as the treatment regimen used. A standardized surgical and rehabilitation protocol, along with long-term care and monitoring, are of critical importance.
The healing and recovery process occurs in stages. In appropriate cases, it is possible to begin controlled weight-bearing in accordance with an established rehabilitation protocol. Full recovery and return to daily activities depend on the patient’s individual condition.
Not every patient is a candidate for a one-stage procedure. In some situations—such as when it is necessary to treat an infection or reconstruct the stump—a two-stage approach is used.
Osseointegration eliminates the need for a denture base, which can significantly improve comfort. However, it still requires proper care, regular medical checkups, and adherence to rehabilitation guidelines.
The patient remains under the constant care of a team of specialists. Regular follow-up visits and monitoring of the adaptation process are an integral part of the treatment.
Osseointegration is not suitable for all amputees. Eligibility for the procedure requires a detailed medical evaluation, including overall health, bone quality, and history of previous treatment. The most common contraindications may include, among others: active infections, insufficient bone quality or length, certain systemic diseases, or situations in which the healing process could be impaired. Therefore, each case is analyzed individually by a team of specialists. Based on imaging studies, medical consultations, and functional assessment, the doctor determines whether osseointegration is a safe and appropriate solution for the patient.