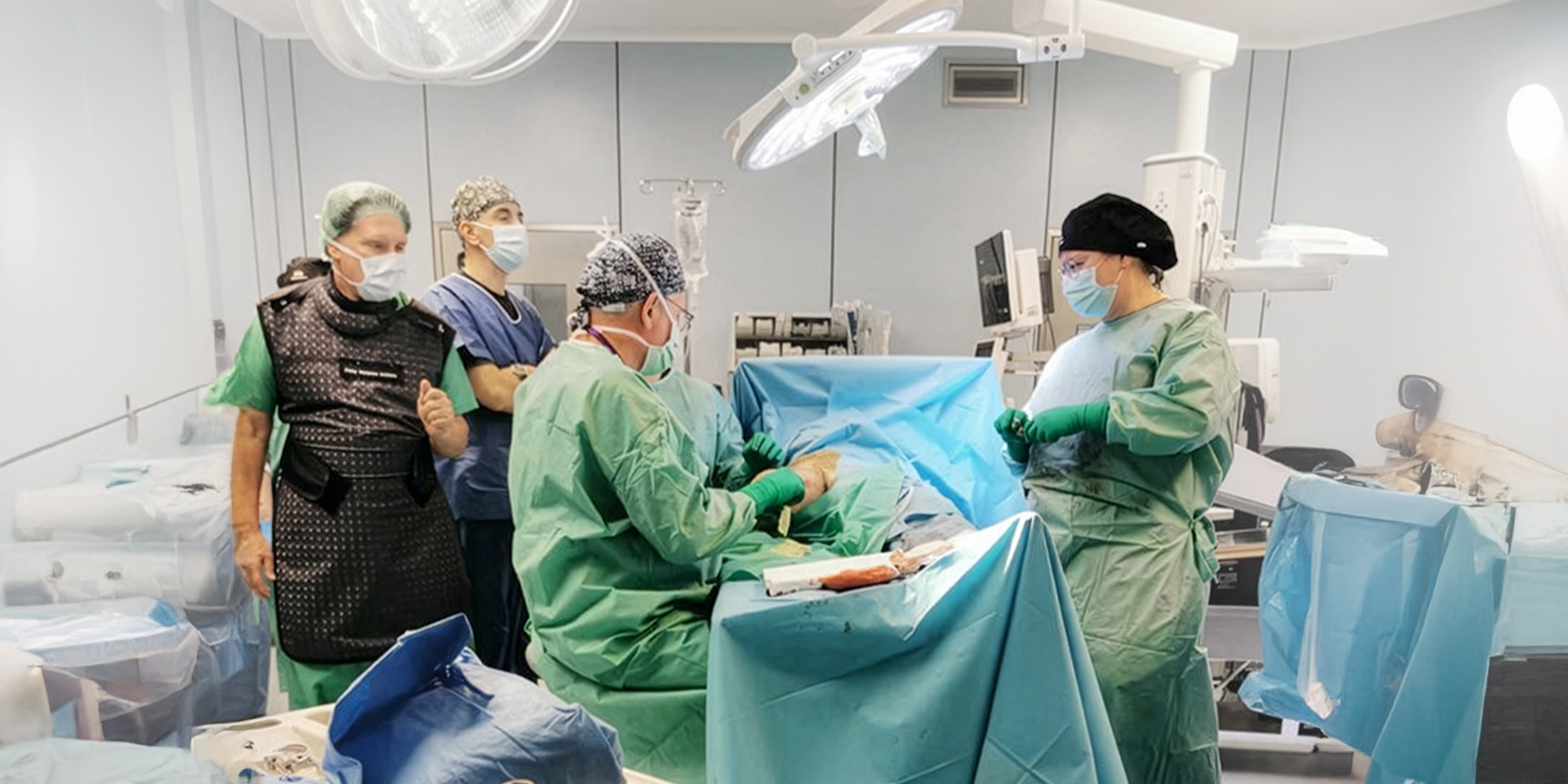
Diagnosis and Treatment Methods for Childhood Cerebral Palsy (MPD).
Children's cerebral palsy (MPD) is a complex condition that requires careful diagnosis and multifaceted treatment. At Paley European Institute, which treats some of the most challenging orthopedic malformations in Europe, we focus on a holistic approach to MPD patients, offering comprehensive care from a variety of specialists and full support for families.
Check:
- Diagnosis of infantile cerebral palsy
- MPD treatment methodology
- MPD treatment - clinical recommendations
- Surgical treatment of MPD
- Holistic approach to treatment at Paley European Institute
- A treatment plan for life
- Summary
Diagnosis of infantile cerebral palsy
Diagnosis of MPD begins with a detailed medical history, physical examination and additional tests. Key steps in the diagnostic process include min:
- Subject examination:
- Prechtel Method: Assessment of spontaneous motility, or analysis of spontaneous movements of the newborn, allowing early detection of the risk of MPD. This method is non-invasive and relies on observation of characteristic movement patterns.
- HINE method: Assessment of a child's motor development, focusing on posture and movements in different positions, which allows identification of possible developmental delays.
- Cortical vision analysis: A study of a child's visual function to assess whether vision problems are due to brain or eye damage. It involves evaluating a child's response to visual stimuli.
Medical history is, for example, pregnancy and birth history, risk factors, medical history
- Neurological examination: Assessment of muscle tone, reflexes, motor coordination and other neurological functions. Neurological testing provides an understanding of how MPD affects a child's nervous system.
- Brain imaging:
- Transcartilaginous ultrasound - a non-invasive examination, without the need for anesthesia, which allows assessment of brain structures. Performed in children in whom the anterior fontanel has not fused (i.e. up to 9 - 18 months of age)
- Magnetic resonance imaging (MRI): Detailed images of the brain help identify areas of damage. MRI is a non-invasive method that provides precise information about brain structure. In smaller children, it must be performed under general anesthesia
- Computed tomography (CT): Helpful in diagnosing bone structures and large brain injuries. CT is often used when fast and accurate results are needed.
- Gait analysis: Use of advanced technology to evaluate a child's gait patterns, which helps in treatment and rehabilitation planning. Gait analysis identifies specific mobility problems.
MPD treatment methodology
MPD treatment requires an individualized approach, tailored to each child's needs and condition. Key treatment approaches include:
- Physiotherapy:
- Exercises to improve muscle strength, flexibility, coordination and balance. Regular physiotherapy prevents contractures and deformities, helping children maintain maximum possible mobility.
- The use of methods such as the Vojta method, Bobath, MEDEK, PNF and many others, which are specialized approaches to the rehabilitation of children with MPD.
- Occupational therapy:
- Developing everyday skills such as dressing, eating and writing. Occupational therapy helps children become more independent.
- Classes aimed at improving hand function and motor coordination, which is crucial for daily functioning.
- Logopedia:
- Speech and language therapy to help children with communication and eating problems. The speech therapist works to improve articulation, language and swallowing skills.
- Using methods like Castillo-Morales to promote speech and eating development.
- AAC - supporting communication with alternative and assistive methods
- Vision Therapy:
- Specialists help improve visual function and adaptation to vision problems. Vision therapy may include exercises to improve eye and hand coordination and visual perception.
- Using specialized tools and techniques to support children with visual problems, which is crucial to their overall development.
- Drug treatment:
- Medications to reduce muscle spasticity, such as baclofen, diazepam or botulinum toxin. Pharmacotherapy helps control symptoms and improves the child's comfort.
- Regular monitoring and adjustment of drug dosages to optimize the effects of therapy and minimize side effects.
- Orthopedic Assistive Devices:
- Bracing, corsets, wheelchairs, verticalizers and other movement and posture aids. These devices help children maintain proper posture and improve mobility.
- Customized hearing aids that are tailored to a child's specific needs for optimal support and comfort.
MPD treatment - clinical recommendations
In treating MPD, it is important to follow recommended clinical standards, which include:
- Early intervention: start therapy as early as possible to take advantage of brain plasticity at a young age. Early intervention significantly increases the chances of improving motor and cognitive functions.
- Multidisciplinary approach: a team of specialists, including neurologists, orthopedists, physiotherapists, occupational therapists, speech therapists, psychologists and vision therapists, work together to develop and implement an individualized treatment plan. Regular meetings of the team make it possible to tailor therapy to the child's needs.
- Regular monitoring and modification of the treatment plan: Constantly evaluating progress and adjusting therapy to the child's changing needs. Regular consultations and examinations allow you to modify the treatment plan on an ongoing basis, ensuring maximum effectiveness.
Surgical treatment of MPD
Surgical treatment of MPD may be necessary in cases where deformities or spasticity significantly limit a child's motor function and daily life. In surgical treatment, the most advanced surgical techniques are :
- Selective dorsal rhizotomy (SDR): A procedure that involves cutting selected nerve roots to reduce muscle spasticity. SDR can significantly improve mobility and quality of life for children with MPD.
- Orthopedic surgeries: Correction of limb deformities, such as soft tissue lengthening, bone osteotomies or joint stabilization. These surgeries are often necessary to improve motor function and prevent further deformities.
- Implantation of baclofen pumps: The insertion of a device that delivers the drug directly into the spinal space, reducing spasticity. Baclofen pumps are effective in controlling spasticity, especially in cases refractory to oral treatment.
- Hip surgery: Treating the risk of hip dislocation, which is a common problem in children with MPD. Regular monitoring and appropriate surgical interventions can prevent serious complications such as pain and loss of motor function.
Holistic approach to treatment at Paley European Institute
At Paley European Institute, we believe that the key to successful MPD treatment is a holistic view of the patient. Every child is different, so our approach is individualized and includes a wide range of specialists:
- Neurologists: Specialists who evaluate and monitor a child's neurological condition.
- Orthopedists: Doctors who treat deformities and bone and joint problems.
- Physiotherapists: specialists in movement therapy.
- Occupational therapists: Experts who help children develop everyday skills.
- Logopedists: Specialists in speech and language therapy.
- Psychologists: psychological support for the child and family, help in coping with stress and emotional challenges.
- Specialists offering functional vision analysis: Specialists assisting children with visual problems.
A treatment plan for life
At Paley European Institute, we create comprehensive treatment plans that cover all aspects of care for a child with MPD throughout his or her life. Families can count on us to help them make medical decisions, giving them comfort and confidence that their child is receiving the best possible care. Thanks to our services, parents don't have to make difficult decisions on their own - we support them in doing so and explain everything thoroughly based on a factual holistic assessment of the child, providing peace of mind and making difficult decisions easier....
Summary
Diagnosis and treatment of childhood cerebral palsy is a complex process that requires the involvement of many specialists. At Paley European Institute, we provide comprehensive care at the highest level, tailored to each patient's individual needs. Our team of specialists works together to provide a holistic approach to treatment, believing that every patient deserves the best care.